Description
A sprained thumb occurs when the ligaments that support the thumb stretch beyond their limits or tear. This usually happens when a strong force bends the thumb backwards, away from the palm of the hand. The most common way for this to occur is by falling onto an outstretched hand.
Most thumb sprains involve the ulnar collateral ligament, which is located on the inside of the knuckle joint. A tear to this ligament can be painful and may make your thumb feel unstable. It may also weaken your ability to grasp objects between your thumb and index finger.
Treatment for a sprained thumb usually involves wearing a splint or cast to keep the thumb from moving while the ligament heals. For more severe sprains, surgery may be needed to restore stability to the joint.
AnatomyHello
Ligaments are strong, fibrous tissues that connect bones to other bones. The ligaments in the thumb help keep the bones in proper position and stabilize the joint.
Sprains can range from a stretch or tiny tear in the fibers that make up the ligament to a complete tear through the ligament or through its attachment to the bone.
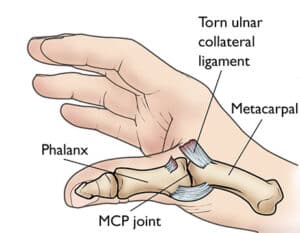
Figure: In this sprain, the ulnar collateral ligament is completely torn.
Grades of Thumb Sprains
Sprains are graded, depending on the degree of injury to the ligaments
- Grade 1 sprain (mild). The ligaments are stretched, but not torn.
- Grade 2 sprain (moderate). The ligaments are partially torn. This type of injury may involve some loss of function.
- Grade 3 sprain (severe). The ligament is completely torn or is pulled off its attachment to the bone. These are significant injuries that require medical or surgical care. If the ligament tears away from the bone, it may take a small chip of the bone with it. This is called an avulsion fracture.
Injury to the Ulnar Collateral Ligament of the Thumb
The most common ligament to be injured in the thumb is the ulnar collateral ligament. This strong band of tissue, which is attached to the middle joint of the thumb (the metacarpophalangeal or MCP joint), keeps your thumb stable so that you can pinch and grasp things.
A sprained thumb is often called a “skier’s thumb” because falling on the ski slopes with your hand strapped to a ski pole is a common cause of injury to the ulnar collateral ligament.
The ligament can also be injured more gradually, over time, from repetitive grasping or twisting activities. This type of chronic injury is known as a “gamekeeper’s thumb.”
The ulnar collateral ligament can tear in different ways. For example, it may be pulled off its attachment at the base of the first bone (the proximal phalanx) in the thumb or from its origin on the metacarpal bone. It can also be torn through its middle, although this is less common.
CausehELLO
Any strong force that bends the thumb backwards, away from the palm of the hand, can stretch or tear the ulnar collateral ligament. This most often occurs by falling onto an outstretched hand.
Sprained thumbs are also common in skiers and in athletes who participate in sports that involve catching and throwing a ball, like football, baseball, and basketball.
SymptomsHello
Depending on the severity of the sprain, pain may or may not occur at the time of the injury. You may have bruising, tenderness, and swelling around the base of your thumb, near the palm.
If the ulnar collateral ligament is completely torn, the end of the ruptured ligament may cause a lump or swelling on the inside of the thumb. Your thumb joint may also feel loose or unstable. You may have difficulty grasping items between your thumb and index finger.

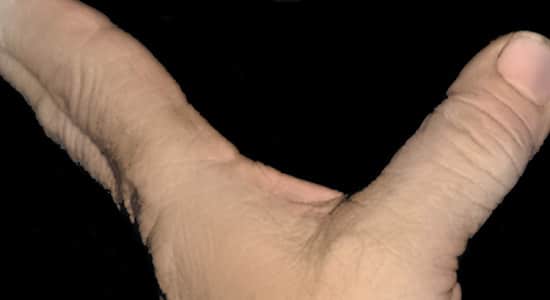
Clinical photo of an unstable thumb. This patient has a complete tear of the ulnar collateral ligament.
Reproduced and adapted from JF Sarwark, ed: Essentials of Musculoskeletal Care, ed 4. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2010.
It is important for your doctor to evaluate even a mild thumb sprain if it does not improve quickly. Proper diagnosis and treatment of a thumb injury is necessary to avoid long-term complications, including chronic pain, instability, and arthritis.
Doctor Examination
Physical Examination
Your doctor will want to know how and when your injury occurred and will ask you to describe your symptoms. He or she will then carefully exam your thumb and hand.
To help determine if the ulnar collateral ligament is partially or completely torn, your doctor will move your thumb in different positions to test the stability of the MCP joint. If the joint is loose and unstable, it is an indication that the ligament may be completely torn.
Imaging Studies
X-rays. X-rays provide images of dense structures, such as bone. Your doctor may order x-rays of your thumb and hand to ensure that you do not have an avulsion fracture or any broken bones. He or she may also take an x-ray of your uninjured thumb to compare it to the injured thumb.
A special type of x-ray, called a stress x-ray, may also be ordered. During this test, your doctor will apply tension to your thumb while it is being x-rayed to learn more about the stability of the MCP joint. If the test causes pain, you may be given an injection of a local anesthetic.
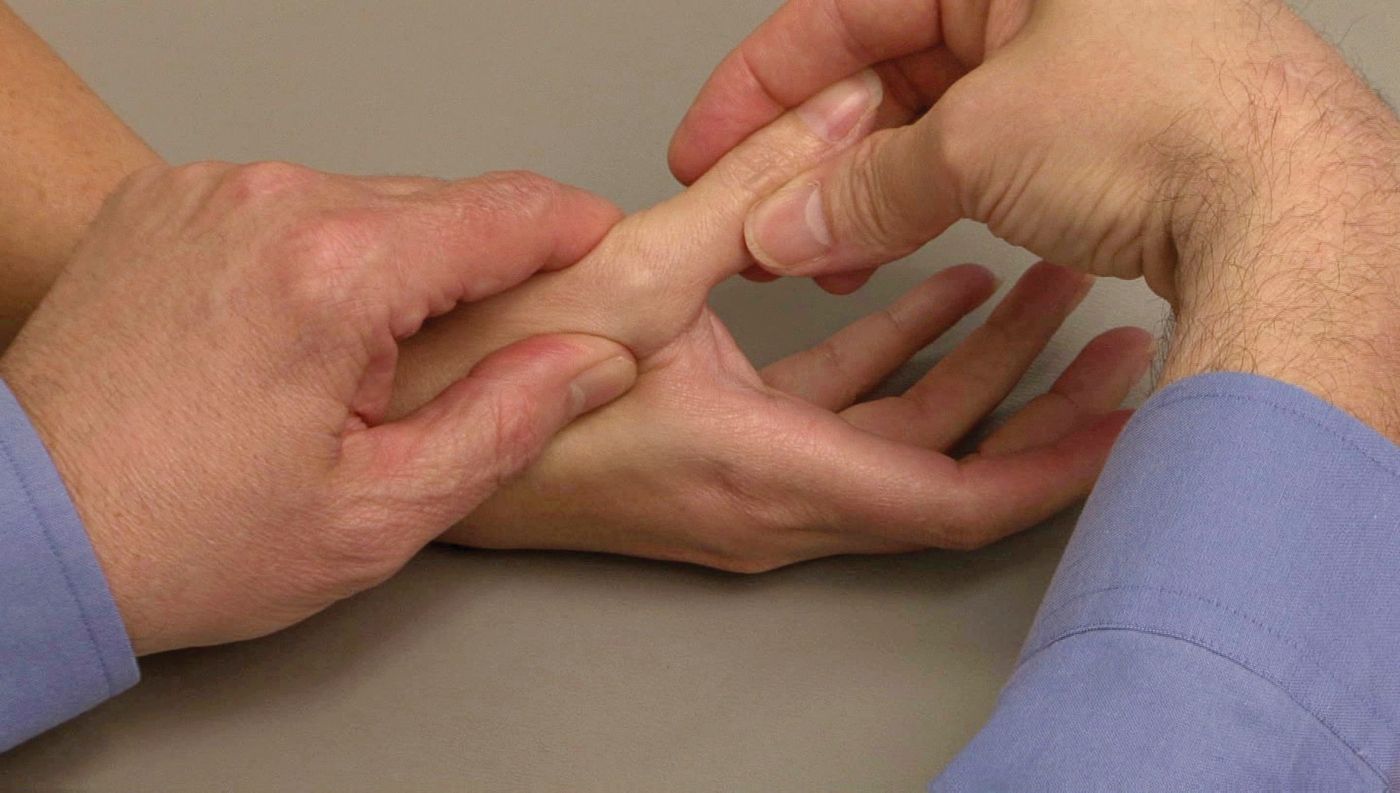
Figure: During a stress x-ray, tension is applied to the thumb to test the stability of the MCP joint.
Reproduced from JF Sarwark, ed: Essentials of Musculoskeletal Care, ed 4. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2010.
Figure: Stress x-ray showing an unstable MCP joint. The abnormal opening of the joint (arrow) is a sign that the ulnar collateral ligament is completely torn.
Other imaging studies.
If more information is needed, a magnetic resonance imaging (MRI) scan or an ultrasound may be ordered. These tests can help your doctor learn more about the severity of your injury and make decisions regarding your treatment and return to activity.
Treatment
Treatment for a sprained thumb depends on the severity of the injury.
Home Care
Mild thumb sprains will usually improve with home treatment that includes the RICE protocol:
- Rest. Try not use your hand for at least 48 hours.
- Ice. Apply ice immediately after the injury to keep the swelling down. Use cold packs for 20 minutes at a time, several times a day. Do not apply ice directly on the skin.
- Compression. Wear an elastic compression bandage to reduce swelling.
- Elevation. As often as possible, rest with your hand raised up higher than your heart.
Additionally, nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin or ibuprofen, can help reduce pain and swelling. If pain and swelling persist for more than 48 hours, however, see a doctor.
Nonsurgical Treatment
For a moderate sprain, your doctor will probably immobilize your thumb joint with a bandage, thumb spica cast, or splint until it heals. To ease pain and swelling, you can apply a cold pack to your thumb twice a day for 2 to 3 days after the injury. Do not apply ice directly on your skin.
Depending on the severity of the injury, you may be instructed to wear the splint or cast at all times. It is important that you avoid applying any pressure or resistance to your thumb until you are permitted by your doctor.
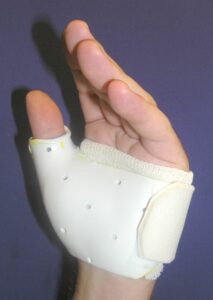
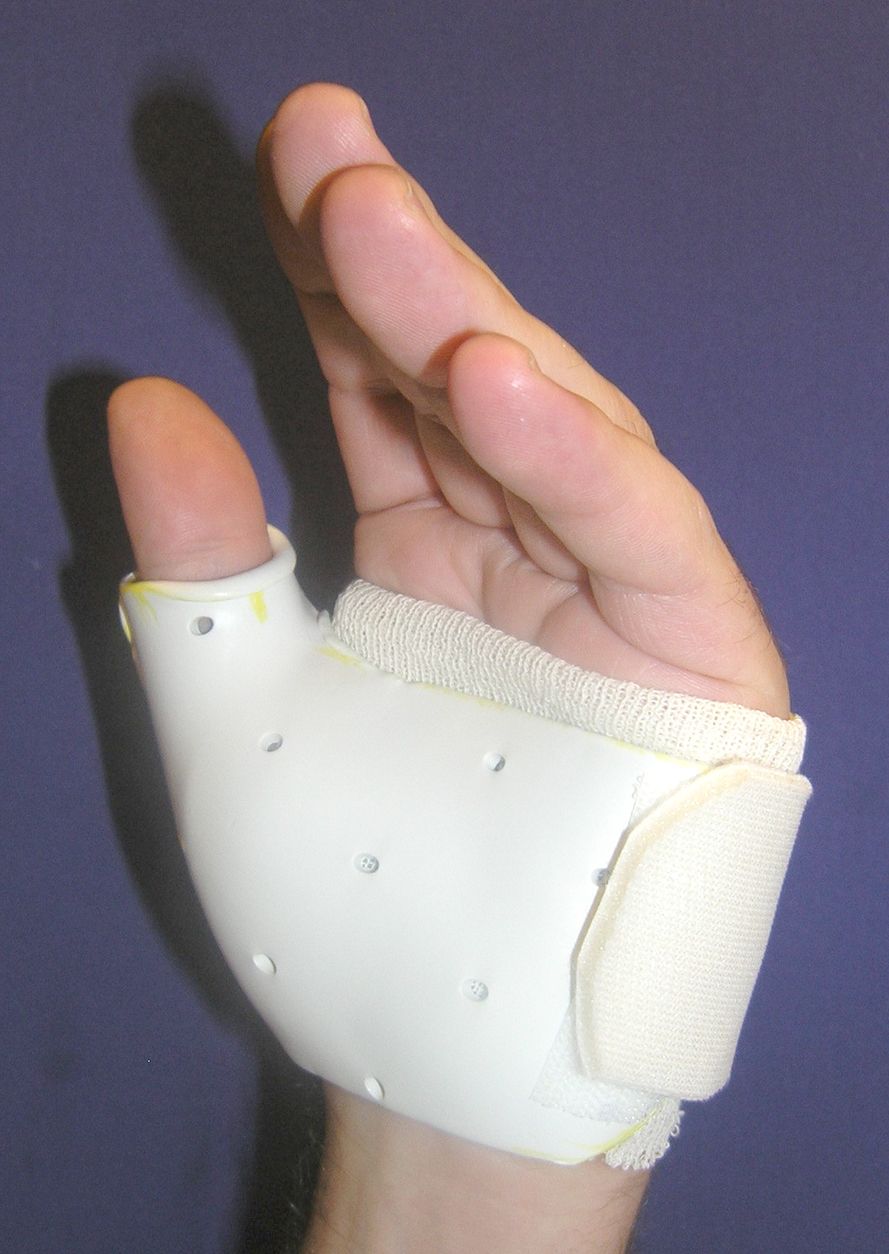
Figure: For a partial tear, wearing a thumb spica cast for a period of time will allow the ligament to heal.
Reproduced from The Sports Medicine Field Manual. Rosemont IL. American Academy of Orthopaedic Surgeons, 2015.
Because immobilization may cause some stiffness in your thumb joint, your doctor may recommend some stretching exercises to help you regain full range of motion.
Surgical Treatment
For a severe sprain, surgery may be needed to restore the stability of your thumb joint and help you regain function. Surgery involves reconnecting the ligament to the bone and/or repairing the avulsion fracture using a pin, screw, or special bone anchor.
After surgery, you may have to wear a short arm cast or a splint for 6 to 12 weeks to protect the thumb ligament while it heals.
Outcomes
When diagnosed and treated properly, most thumb sprains will heal well with no complications. However, a sprained thumb that is ignored with the hope that it will heal on its own may lead to long-term problems, including chronic instability, weakness, and arthritis.
If these late complications develop, surgery may be needed to rebuild the ligament using tissue from your upper arm. If there is significant arthritis, a joint fusion procedure may be needed to address both the arthritis and the instability of the MCP joint.