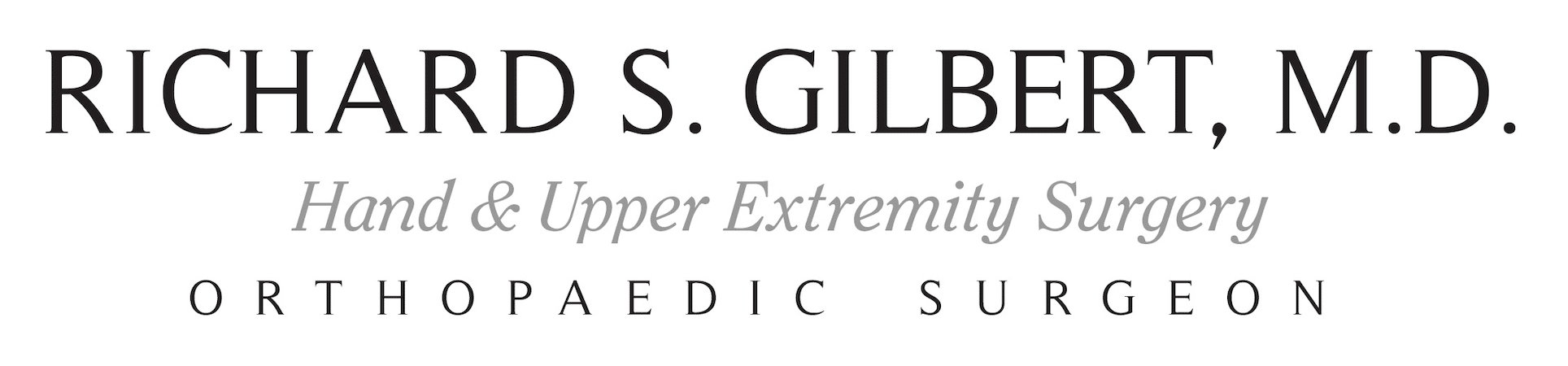Description
A hand infection can cause severe problems that persist even after the infection has resolved, such as stiffness, loss of strength, and loss of tissues such as skin, nerve and bone.
Thus, early and aggressive treatment of infections is essential. When seen early, some types of hand infection can be treated with antibiotics and local rest and soaking. However, many infections begin to cause severe problems, after a day or two, if not treated with antibiotics, surgical drainage, and removal of infected tissues.
Any drainage or pus should be sent for laboratory testing to determine the type of bacteria causing the infection and the appropriate antibiotic for treatment.
Atypical Mycobacterial Infections
Rarely, a hand infection can be caused by an “atypical mycobacterium.” One of the more common types, Mycobacterium marinum infection, can develop after puncture wounds from fish spines or contamination of a simple wound or abrasion from stagnant water (in nature or from aquariums).
These atypical infections develop gradually and may be associated with swelling and stiffness without much pain or redness. Surgical removal of infected tissue may be necessary and is helpful to determine which medicine will help treat the infection; often the medical treatment lasts several months. Patients whose immune systems are not working well (for example, those undergoing chemotherapy or who have HIV) are more susceptible to atypical mycobacterial infections.
Bite Wound Infections
Bacteria from the skin or from the mouth can cause infection in the case of human or animal bites. Thorough washing, soaking, or even surgical drainage of the bite wound is needed to clear the infection, and wounds often are left open so that any infection can drain.
Antibiotics are also used. “Fight bites” to the joint of the hand sometimes result in a chipped tooth being left in the joint; the tooth needs to be removed to prevent infection of the joint. Rabies infection from an animal may be serious or even fatal, so it is important to seek treatment as soon as possible after a bite wound.
Cellulitis
Cellulitis is a skin infection that can cause skin redness, warmth, and pain. People with cellulitis may have a fever or feel sick. Cellulitissually happens around a break in the skin. The infection can spread to the bloodstream and can cause serious problems. Antibiotics are needed right away. Some people need to be admitted to a hospital for treatment.
Deep Space Infections
The hand is divided into many separate “compartments” or “deep spaces.” One or more of these can become infected even from a small puncture wound. An abscess can form in the muscle area at the base of the thumb (thenar space), the palm (deep palmar space), or the web spaces between the fingers. These infections can spread to other areas, even to the wrist and forearm, and need to be drained by surgery.
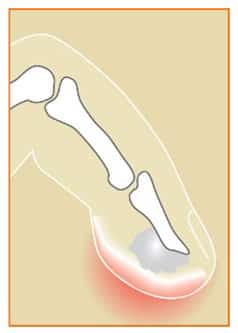
Felon
A painful, throbbing infection of the pulp of the fingertip is called a “felon” (see Figure 1). This closed space is separated into many small compartments, each of which fills with infection and pus. Felon can occur after gardening or other activities that involve sharp objects near the fingertip. Some felons will resolve with soaks and oral antibiotics, but many also need to be drained. If not treated early, destruction of the soft tissues and even bone can occur.
Herpetic Whitlow
Herpetic whitlow is a viral hand infection, usually on the fingers, caused by a herpes virus. This is more commonly seen in healthcare workers whose hands are exposed to the saliva of patients carrying herpes. The condition, characterized by small, swollen, painful blood-tinged blisters, and sometimes numbness, is typically treated conservatively and usually resolves in several weeks without many after-effects.
MRSA
MRSA, or Methicillin Resistant Staphylococcus Aureus, is a bacterium resistant to usual antibiotics used to treat infections. In the past, MRSA was seen in those in a hospital or nursing home. However, MRSA also can come from community places like gyms, dorms, houses, and daycares. Skin infections usually look like boils or collections of pus. Sometimes surgery is needed to drain the infection.
If you start taking an antibiotic for something that looks like this and it is not getting better over two days, contact your health care provider. It is important that skin MRSA is treated right away to prevent it from causing more serious infections. Also, talk to your doctor about what to do to prevent spread to others.
Necrotizing Fasciitis, or Flesh-Eating Bacteria”
Necrotizing fasciitis is a very rare but severe infection. Streptococcus pyogenes or other “flesh-eating bacteria” enter the body through a cut. Bacteria toxins destroy skin, muscles, and other soft tissue. Necrotizing fasciitis is a true emergency—it can be life threatening—and very powerful IV antibiotics are given as soon as possible. Urgent surgery is usually needed to remove dead tissue
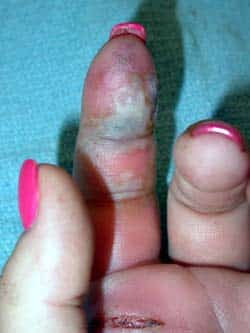
Paronychia
A paronychia is an infection of the paronychium (pay-roh-NIK-ee-um), which is the area around the fingernail (see Figure 2). Paronychia can happen quickly or over time. In acute paronychia, bacteria cause the skin around the nail to be red, swollen, and tender. If the infection is treated early enough, soaks and oral antibiotics may cure the infection. If pus has formed under the skin, surgery to drain the pus is needed. Chronic paronychia is caused by fungus; this usually occurs in people whose hands are frequently wet (such as dishwashers). The cuticle area becomes mildly red and swollen, without drainage and only mild tenderness. This may be treated with special medication and elimination of the constant exposure to moisture, which promotes the fungal infection. Surgery sometimes is needed to remove infected tissue.
Septic Arthritis/Osteomyelitis
A wound in or near a joint can cause septic arthritis, which is a severe infection in the joint. Even a small needle used to drain a cyst at a joint with arthritis can lead to infection. In just days, the cartilage surface of the joint can be destroyed. Urgent surgical drainage and antibiotics are needed. If this treatment is delayed, infection of the bone—called osteomyelitis (ah-stee-OH-my-uh-LIE-tus)—can occur. Septic arthritis with or without osteomyelitis can require one or more surgeries and weeks of intravenous antibiotics.
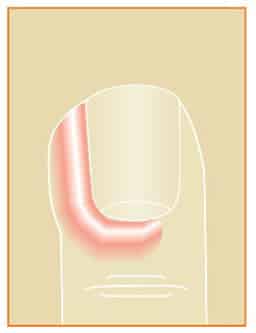
Tendon Sheath Infection(“Infectious Tenosynovitis”)
Tendons that bend the fingers run from wrist, through the palm, up the palm side of the fingers, and to the fingertips. If a small cut or puncture wound occurs in a finger, especially near a joint on the palm side, the canal that the flexor tendon runs through can get infected. This infection can cause severe stiffness or even destroy and pop the tendon. A finger with a tendon sheath infection is swollen, red, and tender over the palm side of the finger, and the finger stays slightly bent and is very painful to extend (see Figure 3). This infection usually requires that the patient be admitted to the hospital for IV antibiotics, soaks, and possible surgical drainage.